WHAT HAPPENS TO A CHILD’S BRAIN WHEN THEY SNORE?
WHAT IS SNORING?
Snoring is a noise that is made when there is either a blockage of airflow, or a disturbance in the normal airflow pattern. Specifically this relates to problems in the breathing somewhere between the nose to the voice box. There are other noises related to noisy breathing, but as snoring is the most common, it is the most important.
ARE KIDS MEANT TO SNORE?
All too often, snoring by kids is ignored by parents. Whilst snoring is normal if it is intermittent, such as when the child is sick with a cold, or is really tired from a busy day of activity, persistent snoring is not normal. We now call persistent snoring habitual if it is present for 4 nights of the week, or more. Habitual snoring is the lesser form of airway obstruction that we collectively call “Sleep Disordered Breathing” or SDB for short. At the worst end of the spectrum of SDB is obstructive sleep apnoea (OSA)- this is where the blockage is so bad that there is no air flowing into the lungs at all-and this is a very bad thing.
CAN WE MEASURE OBSTRUCTED SLEEP?
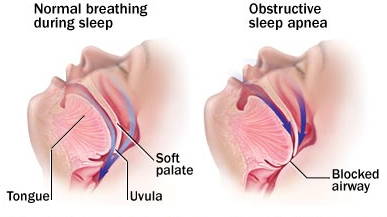
BREATHING AND THE BRAIN
Breathing is an automated process, controlled by the brain. By monitoring chemical levels in the blood, the brain can work out if the breathing is working properly. If the signals to the brain indicate that something is wrong, the brain can alter the rate of breathing to compensate. The problem of airway obstruction though is that even if the brain recognises there is a problem, increasing the effort of breathing achieves very little. Furthermore, blockage to breathing results in oxygen levels in the blood dropping. This is something the brain does not like very much. It triggers off a whole series of problems, which is what this talk is all about.
HOW THE BRAIN WORKS
The brain is incredibly complex. So complex we still don’t fully understand it. But we know the basics. The brain is the control system for the nervous system. For it to work, it needs oxygen- lots of it. If it starts to miss out on oxygen, it quickly panics. This causes all sorts of changes that we can observe and measure. The other important part of the nervous system is to be able to send signals from one place to another. The way these signals are transmitted is via little chemicals. We call these chemical neurotransmitters. And we can measure these also. When we sleep, it is very important that the brain be allowed to work uninterrupted by distractions. Any unsettling events, including low oxygen levels, affect the architecture of sleep in an adverse way.
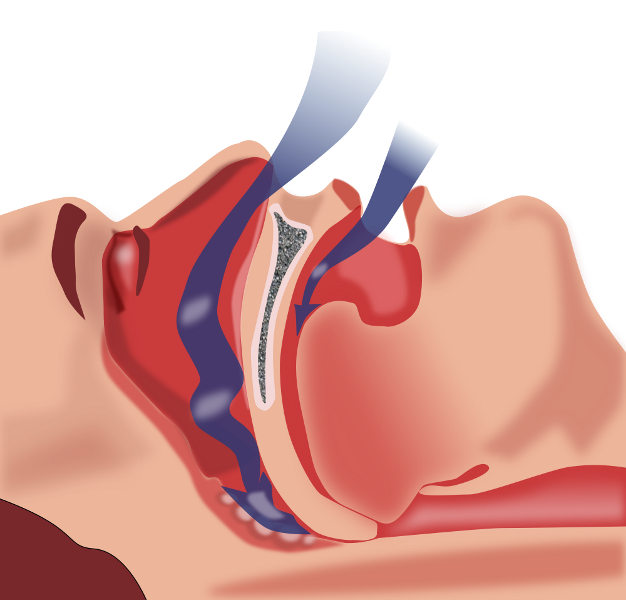
WHAT SORT OF PROBLEMS DO WE SEE?
%
Daytime Sleepiness
%
Cognitive Dysfunctions
%
Memory Problems
%
Problems With Executive Functions
%
Reduced Attention
%
Higher Level of Social Problems
%
Higher Level of Anxiety
%
Higher Level of Depressive Symptoms
BLOOD FLOW TO THE BRAIN
In children that snore, their oxygen levels drop. As a result, the brain needs to make some changes. One of the ways it can try and get more oxygen in is to try and increase the breathing. The other way is to change the flow of blood to the brain. And this is exactly what we have seen happen. Hill CM et al. Pediatrics. 2006 Oct;118(4):e1100-8. Increased cerebral blood flow velocity in children with mild sleep- disordered breathing: a possible association with abnormal neuropsychological function. It is complicated, but the fact that kids with minimal measurable airway obstruction demonstrated changed in the amount of blood being sent to the brain. is an important finding.
BLOOD FLOW TO THE BRAIN AFTER SURGERY
To make things even more interesting, once the airway obstruction is fixed, the blood flow changes resort back to normal levels. So too do the oxygen levels. Hogan AM et al. Pediatrics. 2008 Jul;122(1):75-82. Cerebral blood flow velocity and cognition in children before and after adenotonsillectomy. This study and the previous also showed that children with the snoring and altered blood flow had issues with their brain function, as measured by their ability to think through puzzles and problems. Their concentration also improved once the airway blockages were fixed.
THE EYES- THE WINDOW TO THE SOUL- AND THE BRAIN
It is easier to perform eye tests on adults than kids. By looking into the eye itself, we can actually see the nerves and brain fluid around these nerve. In doing so we have found that in adults with OSA (Obstructive Sleep Apnea), the nerve fibres are damaged, and that the brain fluid pressure is elevated. Xin C et al. Sleep Breath. 2015 Mar;19(1):129-34. Changes of visual field and optic nerve fiber layer in patients with OSAS. These changes decrease the function of the visual system. Claudio L et al. Sleep. 2015 Jul 24. Optic Nerve Dysfunction in Obstructive Sleep Apnea: An Electrophysiological Study.
CHANGES IN BRAIN ACTIVITY WITH OBSTRUCTED BREATHING
We can measure brain wave activity by using special sensors on the head. This is called an EEG. In children with OSA, we can see problems, with the brain wave activity adversely affected. Miano S et al.Sleep. 2009 Apr;32(4):522-9. Prevalence of EEG paroxysmal activity in a population of children with obstructive sleep apnea syndrome. Altered brain activity during the night interrupts a smooth sleep pattern. This seems to translate in to behavioural and mood problems during the day. Aronen ET et al. J Dev Behav Pediatr. 2009 Apr;30(2):107-14. Mood is associated with snoring in preschool-aged children. ADHD is becoming a common diagnosis. It may be that it has a lot to do with sleep.
Children that are inattentive and disruptive may be given the diagnosis of ADHD.
The problem is that children that snore are inattentive also.
ADHD – DID WE GET IT WRONG?
Children that are inattentive and disruptive may be given the diagnosis of ADHD. The problem is that children that snore are inattentive also. Barnes ME et al. Dev Neuropsychol. 2009;34(5):629-49. Impairments in attention in occasionally snoring children: an event- related potential study. They also have problems processing speech, which means their ability to follow instructions is compromised. Key AP et al. Dev Neuropsychol. 2009;34(5):615-28. Sleep-disordered breathing affects auditory processing in 5-7-year-old children: evidence from brain recordings.

When a review of the research on sleep and ADHD was done, 12 studies were identified that had assessed the pre- versus post-surgery ADHD symptoms of children. The results suggested removing the tonsils and adenoids was associated with decreased ADHD symptoms at 2–13 months post-surgery. Sedky K et al. Sleep Medicine Review 2014, 18(4), 349-356. Attention deficit hyperactivity disorder and sleep disordered breathing in pediatric populations: A meta-analysis. So before a diagnosis of ADHD is entertained, sleep disordered breathing in a child should be assessed for first. Fidan T et al. Eurasian J Med. 2008 Apr;40(1):14-7. The impact of adenotonsillectomy on attention-deficit hyperactivity and disruptive behavioral symptoms.
THE BIG STUDY – 11 000 KIDS!
Bonuck K et al. Pediatrics. 2012 Apr;129(4):e857-65.
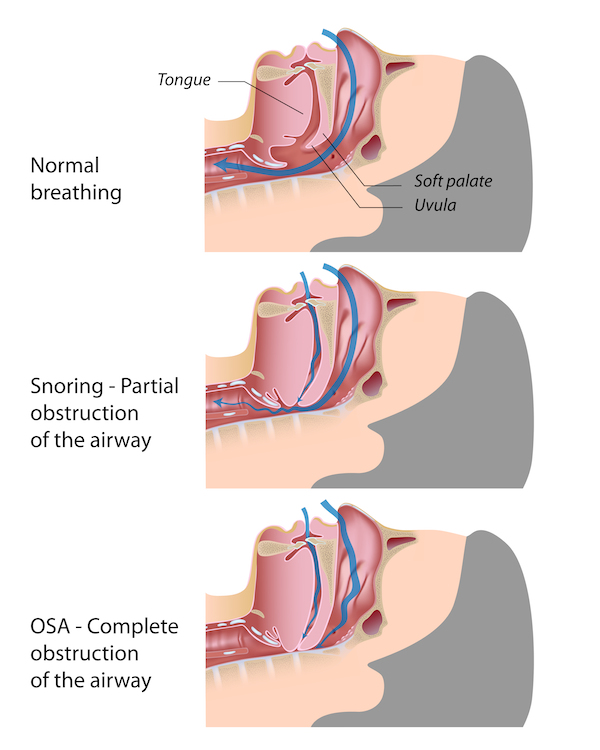
TEETH GRINDING IN KIDS – WHY ARE THEY “STRESSED”?
Grinding the teeth at night is called bruxism. In some children it can be so bad that they can actually crack and chip their teeth. Historically, teeth grinding was thought to be a psychological problem. The issue is that nobody stopped to think why little kids were stressed. What we now know is that in kids who grind their teeth and who have an airway problem, once the airway problem is fixed, 80% of them also stop grinding their teeth. They are stressed becuase they can’t breathe properly. Eftekharian A et al. Int J Pediatr Otorhinolaryngol. 2008 Apr;72(4):509-11. Bruxism and adenotonsillectomy. DiFrancesco RC et al. Int J Pediatr Otorhinolaryngol. 2004 Apr;68(4):441-5. Improvement of bruxism after T & A surgery.
TEETH GRINDING AND LOW OXYGEN LEVELS
With teeth grinding being the most obvious form of abnormal jaw movement due to the noise made as the teeth clash against each other, there are also subtle jaw movements that we can measure. Interestingly, these small movements seem to relate to intermittent low oxygen levels. Dumais IE et al. J Oral Rehabil. 2015 Jul 1. Could transient hypoxia be associated with rhythmic masticatory muscle activity in sleep bruxism in the absence of sleep-disordered breathing? A preliminary report. Teeth grinding also seems to tie in with changes in blood pressure. We will come back to mentioning blood pressure later on. Nashed A et al. Sleep. 2012 Apr 1;35(4):529-36. Sleep bruxism is associated with a rise in arterial blood pressure.
CHANGES IN BRAIN TRANSMITTERS
In bruxism, we can see changes in the levels of neurotransmitters. This includes serotonin and dopamine. Mayer P et al. Chest. 2015 Jul 30. Sleep Bruxism in Respiratory Medicine Practice. These neurotransmitters are also implicated in depression. And sleep disordered breathing is implicated in depression and other psychological problems in kids. Lee CH et al. Int J Pediatr Otorhinolaryngol. 2014 Dec;78(12):2145-50. Psychological screening for the children with habitual snoring.
MOUTH BREATHING- NOT AS GOOD AS THROUGH THE NOSE
Although the air drawn in to the body is the same, there is a big difference as to whether it comes via the nose or the mouth. In mouth breathing, which occurs w=in children when the nose is blocked, the blood oxygen levels drop. This causes all the problems mentioned so far, even if they don’t snore. Niaki EA et al. Acta Med Iran. 2010 Jan-Feb;48(1):9-11. Evaluation of oxygen saturation by pulse-oximetry in mouth breathing patients.
AND IT’S NOT JUST THE BRAIN THAT SUFFERS
Apart from all the problems with brain function, sleep disordered breathing in children also has adverse effects on the heart and blood pressure. Walter LM et al. Sleep Breath. 2013 May;17(2):605-13. Autonomic dysfunction in children with sleep disordered breathing. In fact, it may very well be that the high blood pressure experienced in adulthood stems from sleep problems as a child. Vlahandonis A et al. Sleep Med Rev. 2013 Feb;17(1):75-85. Does treatment of SDB in children improve cardiovascular outcome? And many children are not being treated appropriately. Nisbet LC et al. Sleep Med Rev. 2014 Apr;18(2):179-89. Blood pressure regulation, autonomic control and sleep disordered breathing in children.
THE CONSEQUENCES OF POOR SLEEP OVER TIME
Poor sleep adds up over time. In this study, the chances of developing dementia increased as the sleep quality decreased. Tsapanou A et al. Dement Geriatr Cogn Dis Extra. 2015 Jul 10;5(2):286-95. Daytime Sleepiness and Sleep Inadequacy as Risk Factors for Dementia. There are many causes for a bad night’s sleep. And one of them is sleep apnoea. Gagnon K et al. Pathol Biol (Paris). 2014 Oct;62(5):233-40. Cognitive impairment in obstructive sleep apnea.
BRAIN SCANS AND POOR MOTOR SKILLS
Believe it or not, we now have the technology to measure brain function. We can also measure the size of the brain. In kids with sleep disordered breathing, the parts of the brain responsible for thinking, conflict resolution, and attention are struggling to perform. Kheirandish-Gozal L et al. Sleep. 2014 Mar 1;37(3):587-92. Preliminary functional MRI neural correlates of executive functioning and empathy in children with obstructive sleep apnea. Furthermore, these kids have smaller brains and problems with their fine motor skills. Chan KC et al. Sleep Med. 2014 Sep;15(9):1055-61. Neurocognitive dysfunction and grey matter density deficit in children with obstructive sleep apnoea.
OSA AND ALZHEIMER’S DISEASE
Alzheimer’s disease is the most common cause of dementia. It is characterised by a build up of protein in the brain called amyloid. It is though that this build up affects the communication system within the brain. In studies of mice, where their oxygen levels were decreased, their brains started to show a build up of amyloid. Daulatzai MA. Neurotox Res. 2013 Aug;24(2):216-43. Death by a thousand cuts in Alzheimer’s disease: hypoxia–the prodrome.
%
How Big is The Problem?
HOW BIG IS THE PROBLEM?
More than 25% of all children, not just those with ADHD, will have a sleep disorder at some point. These have enormous and varying impacts on family dynamics, school success and other health issues.
SO WHAT’S NEXT?
Children are not supposed to snore
Specialist Review
Take Action



